Surprising Truths About Male Pelvic Health That No One Talks About
Introduction: Beyond the Basics
For most men, the "pelvic floor" is unfamiliar territory. If it's mentioned at all, it's typically in the context of problems like incontinence after prostate surgery. But this view is incredibly limited. These muscles are not just about preventing leaks; they play a vital role in everything from sexual health to chronic pain.
This article is a journey to uncover the surprising and essential functions of the male pelvic floor. We will reveal five of the most impactful, counter-intuitive, and rarely discussed facts about male pelvic health, empowering you with the crucial knowledge to better understand your body and advocate for your well-being.
1. That Nagging "Prostatitis" Might Not Be Your Prostate at All
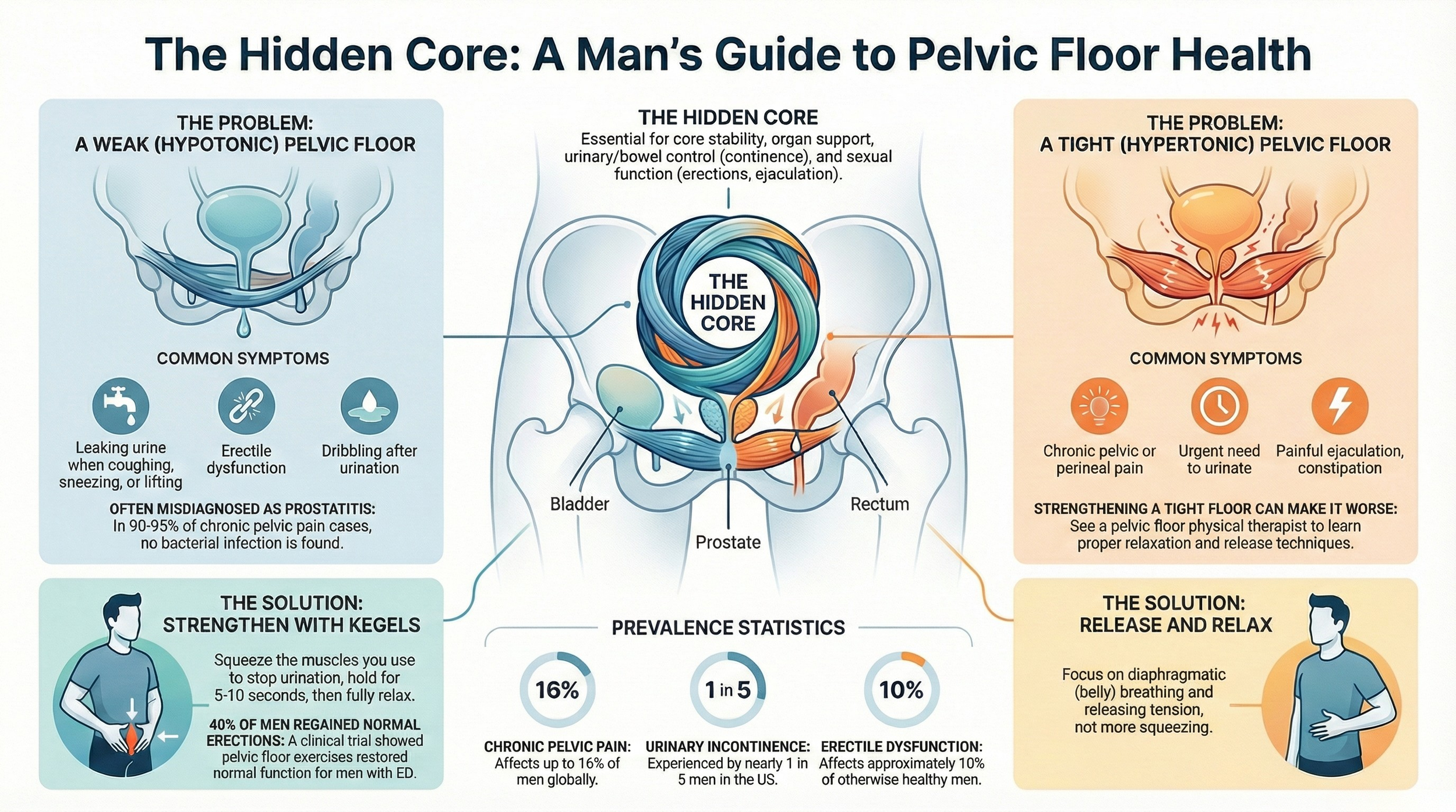
One of the most common diagnoses for persistent male pelvic pain is Chronic Prostatitis/Chronic Pelvic Pain Syndrome (CP/CPPS), but this name is often misleading. The surprising truth is that approximately 97% of men with these symptoms do not actually have any pathology or infection in their prostate gland.
Instead, studies show that up to 90% of these men have pelvic floor muscle and girdle dysfunction. This is a critical distinction. Misdiagnosing the issue as a prostate infection can lead to multiple, ineffective rounds of antibiotics, leaving the root cause—muscle tension and dysfunction—unaddressed. Understanding that the pain likely originates in the surrounding muscles guides men toward effective treatments like pelvic floor physical therapy, which can provide lasting relief.
2. Your Pelvic Floor Is a Major Player in the Bedroom
The pelvic floor's function extends far beyond bladder and bowel control; it is a crucial component of male sexual health. In fact, the same pelvic floor muscle dysfunction that can be misdiagnosed as prostatitis is also a primary culprit in the bedroom, affecting everything from erection to ejaculation. Specific muscles in this region have distinct roles in sexual function:
The bulbospongiosus muscle is important for ejaculation and for expelling the last drops of urine.
The ischiocavernosus muscle helps to maintain an erection.
When these muscles are weak, it can be a direct cause of sexual dysfunction, including erectile dysfunction and leaking urine with orgasm (climacturia). The connection is significant: a large-scale meta-analysis found that 59% of men with CP/CPPS experience some form of sexual dysfunction, with a 34% rate of erectile dysfunction and a 35% rate of premature ejaculation. This knowledge shifts the perception of pelvic floor health from just "preventing leaks" to enhancing a vital aspect of a man's life.
3. Chronic Pelvic Pain Is a Brain-Body Disorder
The modern scientific understanding of chronic pelvic pain reveals it's not just a localized muscular issue but a complex brain-body disorder. This is often driven by a phenomenon called "central sensitization," where the central nervous system becomes persistently over-reactive, amplifying pain signals. Think of it like a car alarm that has become too sensitive—it goes off not just when someone is breaking in, but when a leaf falls on the windshield. In the same way, the nervous system begins to interpret normal signals from the pelvic region as pain.
A 2025 study published in Frontiers in Neuroscience provided objective proof of this connection. Using advanced neuroimaging, researchers found functional alterations in the brains of patients with CP/CPPS. The specific brain regions implicated included:
Anterior cingulate cortex (ACC)
Amygdala
Insula
Thalamus
These areas are all known to be involved in pain processing and emotional regulation. This is an impactful discovery because it provides biological evidence that validates the patient's experience of pain. It also supports a more integrated treatment approach that combines pain neuroscience education with physical therapy to address both the brain and the body.
4. "Success" After Incontinence Surgery Isn't Always Being 100% Dry
For men with moderate to severe stress urinary incontinence (SUI), often following prostate surgery, the Artificial Urinary Sphincter (AUS) is considered the "gold standard" treatment. For mild to moderate cases, a male sling is often used. These procedures have high satisfaction rates, with 90% of AUS patients reporting satisfaction and 96% saying they would recommend it to a friend.
However, a crucial and counter-intuitive truth is that "success" is often a negotiation between the patient and the doctor. The goal is not always to be 100% dry. As Dr. Gregory Lowe explains, the aim is often to become "socially continent," which he defines as returning men to using one to two pads per day. This is considered a major victory because it allows men to return to an active life—playing golf, exercising, and working—without the constant fear of wet pants. The true measure of success is this return to normalcy and confidence.
It is also important for patients to have realistic expectations. As Dr. Lowe notes from his clinical observation, even these effective devices can be overcome if the bladder is allowed to fill completely. This means a man may need to continue to plan bathroom breaks and wear a pad for "security," as leaks are still possible if he waits too long. Despite the nuances of what constitutes "dryness," patient satisfaction with these procedures is overwhelmingly high, a fact confirmed in multiple clinical studies.
5. Prostate Removal Changes Orgasm in a Way Few Expect
A radical prostatectomy is a life-saving surgery for many men, but it comes with a significant side effect that is often undiscussed. During the procedure, the prostate gland and the seminal vesicles are completely removed. Because these organs produce semen, men who undergo this surgery will no longer produce any ejaculate.
It is critical to understand that men can still achieve orgasm, but it will be a "dry orgasm" without any fluid. This is a direct anatomical result of the surgery, where the prostate and seminal vesicles are removed, and the bladder is then reconnected directly to the urethra, bypassing the structures that once produced and transported semen. Proper pre-surgical education on this topic is essential, as it allows men and their partners to understand, prepare for, and adapt to this permanent change in their sexual experience.
Conclusion: A Call for Conversation
The male pelvic floor is a complex and critical area that impacts a man's quality of life far beyond bladder control. From sexual function to chronic pain, its health is integral to overall well-being. Understanding these hidden truths can empower men to ask better questions, challenge misdiagnoses, and advocate for the right kind of care.
Given how central these muscles are to daily life and well-being, isn't it time we started talking about male pelvic health before it becomes a problem?